Almost everyone has heard of varicose veins. In most people, this vascular disease is associated with problems with the legs, but quite often the pelvic organs become the place of localization of the pathological process. One of the types of this pathology is varicose veins of the uterus.
The disease is diagnosed mainly in women or girls who have entered childbearing age, but in some cases it also develops in adolescent girls. To cope with the pathology, it is important to know the main causes and symptoms of its occurrence, as well as to have an idea of the methods of treatment.
Features of pathology
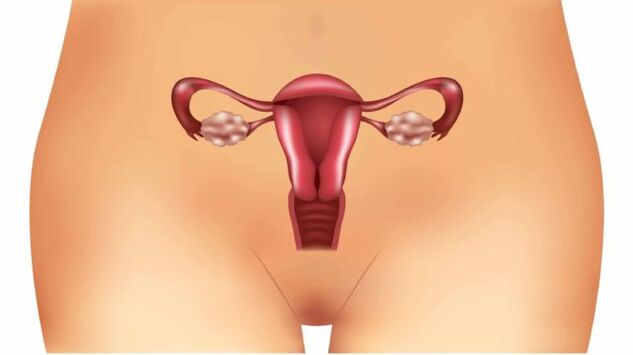
Varicose veins of the uterus, what is it? This medical term refers to a disease caused by a number of pathological factors affecting the venous network of the pelvic organs:
- Thinning of the vascular walls.
- The formation of vascular nodules.
- Expansion of the venous lumen.
These three factors negatively affect the process of blood circulation in a separate part of the organ and lead to valvular insufficiency of the veins in the same area. The disease is difficult to diagnose due to the absence of obvious clinical signs, as well as the similarity with diseases of the pelvic organs of an inflammatory nature. For these reasons, the pathology is often detected in severe stages, when its treatment is much more complicated.
Gynecologists distinguish two subspecies of the pathological process:
- Varicose veins of the uterus.
- Varicose veins of the cervix.
In any case, the disease is dangerous for its complications, among which there are inflammatory processes that cover the uterus, ovaries and vagina. The most serious complication is infertility.
Causes of disease
Understanding the factors underlying disease development offers several key benefits. First, it allows the doctor to diagnose faster and more accurately, as well as prescribe adequate treatment. Secondly, a woman will be able to try to prevent the development of pathology.
Consider the most likely causes of uterine varices:
- Pregnancy is considered the main factor in the development of the pathological process. Already at the embryonic stage, then as the fetus grows and develops, uterine circulation increases (it all depends on the period). At the same time, in vessels with a weakened venous wall, valve function is disturbed and they are stretched. In addition, a growing fetus increases the load on the pelvic organs, which can also give impetus to the development of the disease.
- Take hormonal drugs for a long time. Specific drugs negatively affect the condition of the vessels, their walls lose their elasticity.
- Another factor that provokes the disease is reduced motor activity. A sedentary or sedentary lifestyle leads to a decrease in the contractile function of the muscles, the consequence will be a violation of blood circulation.
- Increased physical activity on the pelvic region. In this case, as during pregnancy, blood flow to the pelvic organs, especially to the uterus, increases.
- Increased constipation - in this case, the cause of varicose veins again becomes increased blood flow. However, circulation is now increased due to increased intra-abdominal pressure.
- Congenital anomalies of the structure of the uterus.
- Artificial termination of pregnancy.
- Difficult childbirth.
- Inflammatory processes in the pelvic organs.
Symptoms and Diagnosis
The complexity of diagnosing uterine varices lies in the fact that the symptoms of this disease are masked like other pathologies. In addition, the clinical picture indicating the development of the disease is rather poor:
- Frequent pain, recurring more than 3-4 times a week in the lower abdomen, closer to the pubic region. The pain syndrome is pronounced, the nature of the pain pulls and hurts. In some cases, the pain is so intense that the woman loses her ability to work, it is even difficult to get out of bed.
- More than 80% of women with uterine varices feel discomfort or even pain during or after sexual intercourse.
- Violation of the menstrual cycle, delays in menstruation up to 50-60 days are possible. In this case, the discharge is often scanty, the menstruation stretches for 5-7 days. The prolonged absence of periods in many women is considered the first sign of menopause.
This clinical picture is inherent in a number of other gynecological diseases. For this reason, it is impossible to make a diagnosis solely on the basis of symptoms, the doctor is obliged to prescribe a number of diagnostic measures. Also, in varicose veins of the cervix, the symptoms are about the same.
Important: Varicose veins of the uterus are diagnosed mainly at the second stage, since it is then that the described symptoms begin to disturb the woman. The earlier the pathology is detected and its treatment started, the lower the risk of complications, in particular infertility.
As for direct assignment studies, they are as follows:
- Ultrasound, which is performed by the transvaginal method.
- CT of the pelvic organs.
- Dopplerography.
- Selective ovaricography.
The need for each diagnostic method depends on the data obtained as a result of ultrasound, since it is carried out first.
Features of the disease during pregnancy
Due to the increased load on the body as a whole and the pelvic organs, during pregnancy the risk of developing uterine varices increases. Until a woman gives birth, the disease is not treatable.
The pathology that develops during pregnancy affects the choice of mode of delivery. Very often, the doctor decides to perform a caesarean section. This is done in order to avoid complications in the form of thrombophlebitis, internal bleeding, thrombosis, etc.
Regardless of the period of pregnancy during which the disease was detected, a woman should be constantly monitored by a doctor to monitor the condition of the fetus and the progression of varicose veins.
Important: When planning a pregnancy, have an exam to identify uterine varices and other gynecological problems. This will help to avoid complications during childbirth and reduce the risk of pathologies of fetal development.
Disease treatment
To receive qualified assistance with varicose veins, you need to contact a doctor, first a gynecologist, who will then refer you to a phlebologist.
The mainstay of treatment is drug therapy, which consists of taking the following drugs:
- Venotonics - drugs of this group have a beneficial effect on the condition of blood vessels. They tone capillaries and blood vessels, reduce their permeability, increase elasticity and strengthen the walls of veins.
- Drugs to reduce blood viscosity - contribute to a general improvement in the inflow and outflow of blood from the affected vessels, reduce the risk of thrombosis. Means of this group are contraindicated in pathologies of the cardiac system.
Important: Any medicine is prescribed only by a doctor, based on a preliminary diagnosis, the patient's medical history and taking into account the stage of development of the disease. It is important to pay particular attention to women in office.
Treatment methods
In addition to pharmacotherapy for comprehensive treatment, an integrated approach and implementation of the following recommendations are important:
- compliance with the sleep regime;
- minimize physical activity, but at the same time maintain mobility;
- follow a diet that includes plenty of vegetables, fruits, and vitamin E-rich oils;
- support sports, therapeutic gymnastics;
- complete exclusion of any bad habits;
- some doctors recommend doing Kegel exercises, which help strengthen the vaginal muscles.
Surgical intervention
Such drastic measures are necessary in cases where conservative treatment did not give good results or the disease was detected at a late stage. The following methods of surgical intervention are the most popular:
- Phlebectomy is the removal of individual sections of small vessels.
- Laser coagulation is the most sparing type of restoration of normal blood flow.
- Sclerotherapy is the introduction into the cavity of a vein of an agent that promotes its sticking. The lack of blood supply in the vessel will lead to its spontaneous elimination.
- In the most severe cases, it is necessary to carry out a complete removal of the uterus, sometimes with the appendages.
ethnosciences
Alternative methods are one of the options for complex treatment in a conservative manner. They are not able to completely replace drug treatment, but can affect the success of treatment in general.
The most effective means of traditional medicine are:
- Horse chestnut infusion: take 100 grams of horse chestnut, chop them with the skin. Pour the resulting raw material with such an amount of vodka that it covers the crushed fruit by 4-5 millimeters. Insist in a dark place for 14-15 days. After that, the infusion is taken 10 drops twice a day. The tool strengthens the vascular walls and thins the blood.
- Lilac tincture: for 0. 5 liters of vodka it is necessary to take 100 grams of lilac flowers and 30 grams of propolis. All ingredients are poured with vodka and left in a dark place for 30 days (every 2-3 days you need to shake). Then the tincture is filtered and consumed 15 milliliters three times a day before meals.
Do not forget that before using even the most harmless traditional medicine, you should consult a doctor.
Complications of the disease
Varicose veins of the uterus are dangerous for their complications in the absence of adequate treatment. These complications are as follows:
- internal bleeding;
- thrombosis;
- inflammatory processes in the genitals;
- Menstrual irregularities;
- hormonal dysfunction of the ovaries;
- infertility.
Preventive measures
It is always better to carry out the prevention of a disease, preventing its development, than to deal with it or its consequences later. To prevent uterine varices, follow these simple guidelines:
- lead a mobile life, walk more and walk;
- doing gymnastic sports;
- eat healthy, less fatty, fried, spicy, spicy, sour foods;
- make regular appointments with the gynecologist, especially at the slightest complaint.

Despite the difficulties in detecting varicose veins of the uterine veins, in order to avoid disease progression and complications, if the previously described symptoms appear, consult a doctor. It is also important to remember that self-treatment in such cases is contraindicated, careful diagnosis and constant monitoring by a gynecologist and phlebologist are required.












































